Yes, there is a real, specific test for bird flu in humans. Clinicians use RT-PCR (reverse transcription polymerase chain reaction) with H5-specific primers and probes to detect avian influenza A(H5N1) in respiratory specimens. This is not something you can do at home or order yourself online. The process runs through your doctor, your state public health department, and in some cases, the CDC. But if you have genuine exposure and symptoms, the system is designed to move quickly, and you will not be left guessing.
How to Test for Bird Flu in Humans: Diagnosis Guide

Is there a test for bird flu in humans?
There is, and it is more targeted than a standard flu test. The gold-standard method is RT-PCR using H5-specific primers and probes, run at state or local public health laboratories. This test looks specifically for the genetic fingerprint of avian influenza A viruses, particularly HPAI A(H5N1). A regular rapid flu test at a pharmacy or urgent care clinic cannot distinguish bird flu from seasonal flu. It might detect that you have influenza A, but it cannot tell you which subtype. That distinction matters enormously, which is why standard clinical labs refer confirmed influenza A positives to public health labs for subtyping using the CDC Influenza A Subtyping kit.
Beyond PCR, confirmation can also involve virus isolation in specialized biosafety labs and, in cases where the acute illness has passed, serological testing. The WHO case definition allows for laboratory confirmation via positive PCR, virus isolation, or serology. Serology is typically a backup, used when someone was exposed weeks ago and did not get tested during the acute phase. A single convalescent serum sample collected at least 21 days after symptom onset or exposure showing a neutralizing antibody titer of 1:40 or higher to an influenza A(H5) virus can support a positive serological finding.
When to suspect it: symptoms and exposure that trigger testing

Testing is not triggered just by symptoms alone. Public health guidance is clear that both an epidemiologic link AND clinical presentation are required before testing is initiated. Think of it as two keys that both need to turn at the same time.
On the exposure side, the scenarios that raise a red flag include direct or close contact with infected or potentially infected poultry or wild birds, contact with sick or dead birds during a known outbreak, working on or visiting a farm with confirmed HPAI, handling raw poultry or bird products in a high-risk setting, or close unprotected contact with a confirmed or suspected human case. Dairy farm workers exposed to infected cattle herds have also been flagged in the current outbreak context, given H5N1's documented presence in cattle since 2024.
On the symptom side, bird flu in humans typically presents with fever, cough, sore throat, and shortness of breath, which can progress to pneumonia and severe respiratory illness. Conjunctivitis (pink eye) has been a notable presentation in some H5N1 cases, particularly among people with direct exposure to infected animals. Gastrointestinal symptoms like nausea, vomiting, and diarrhea have also been reported. If you have eye symptoms only and a relevant exposure history, that still warrants evaluation. CDC specifically recommends collection of both a conjunctival swab and a nasopharyngeal swab for anyone presenting with conjunctivitis following a relevant exposure.
How clinicians evaluate you before testing
Before any swab is collected, a clinician will run through a structured risk assessment. This is essentially an interview combined with a clinical exam, and it has two goals: figuring out whether you genuinely need bird flu testing (rather than standard flu testing), and making sure the right precautions are in place before specimens are collected.
The exposure history is the most critical piece of this evaluation. A clinician will ask about your occupation, recent animal contact, travel, and whether you have been near confirmed outbreak locations. They will also assess the timing, because the window between exposure and testing matters for viral shedding levels.
Importantly, clinicians are instructed by CDC to contact the state health department before or while arranging testing. This is not a formality. The state health department helps coordinate the logistics, confirms that the right public health lab is used, and ensures the specimen gets processed with the correct assay. It also triggers the public health response machinery if needed. If you show up to a hospital or clinic with a credible exposure history and compatible symptoms, expect your provider to make that call fairly quickly. In the meantime, you may be placed in a room away from other patients to reduce any potential exposure risk, and the clinical team will use appropriate personal protective equipment during specimen collection.
For asymptomatic individuals with high-risk exposures, testing is still possible. CDC guidance notes that when feasible, asymptomatic people with significant exposure may receive a nasal or oropharyngeal swab, plus a conjunctival swab if relevant, in consultation with the health department. So even if you feel fine but had a significant exposure, it is worth a call to your local health department.
Which tests are used and what specimens are collected
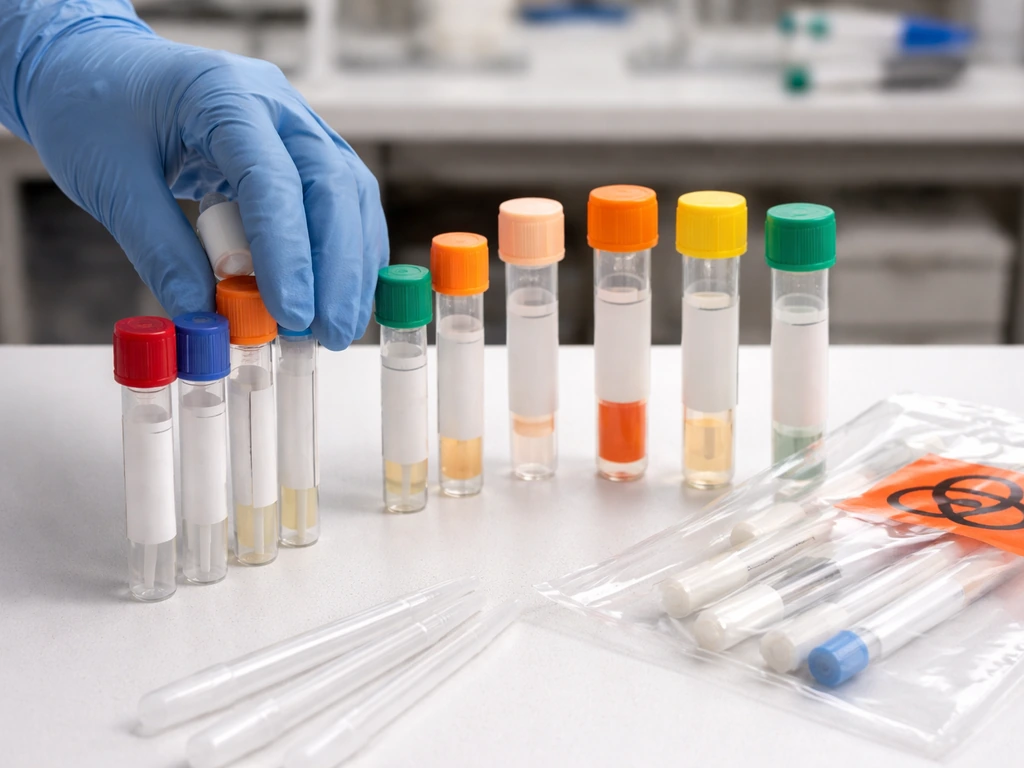
The main diagnostic test is RT-PCR with H5-specific primers and probes. This is a molecular assay that detects viral RNA directly from your specimen. It is highly sensitive and specific for avian influenza subtypes when run with the right reagents at a qualified public health lab.
Rapid influenza diagnostic tests (RIDTs) of the kind used in most urgent care clinics detect influenza antigen, not the specific subtype. They can flag that you have influenza A, which is a useful first signal, but they cannot confirm or rule out H5N1. RT-PCR is the method that actually matters for bird flu diagnosis.
For specimen collection, the priority upper respiratory sample is a nasopharyngeal swab, wash, or aspirate. Nasopharyngeal specimens have higher yield than nasal or throat swabs alone. Combined nasal and throat swabs are also acceptable, and importantly, CDC recommends that the nasopharyngeal swab and the combined nasal-throat swab be tested separately rather than pooled together. If you only have conjunctivitis and no respiratory symptoms, a conjunctival swab can be used with the CDC Influenza A/H5 assay, ideally alongside a nasopharyngeal swab when possible.
| Specimen type | When it's used | Test method |
|---|---|---|
| Nasopharyngeal swab/wash/aspirate | First choice for most patients with respiratory symptoms | RT-PCR (H5-specific) |
| Combined nasal and throat swabs | Acceptable alternative; tested separately | RT-PCR (H5-specific) |
| Conjunctival swab | Patients with conjunctivitis, with or without respiratory symptoms | CDC Influenza A/H5 assay |
| Endotracheal aspirate or BAL fluid | Critically ill patients on ventilation who tested negative on upper respiratory specimens | RT-PCR |
| Sputum | Lower respiratory involvement; used alongside or after upper respiratory specimens | RT-PCR |
| Paired acute/convalescent serum | Used retrospectively when acute testing was missed; 21+ days post-exposure | Neutralization serology |
For patients who are critically ill and on mechanical ventilation and have already tested negative on an upper respiratory specimen, CDC recommends collecting a lower respiratory specimen, either an endotracheal aspirate or bronchoalveolar lavage (BAL) fluid. This is because H5N1 and H7N9 can have prolonged viral shedding in the lower respiratory tract in severe cases, meaning the upper airway sample may miss the virus even when it is still present and detectable lower down.
How the testing process works: from sample to confirmation
Once specimens are collected, they go to a state or local public health laboratory, not a commercial lab. The public health lab runs the CDC Influenza A Subtyping kit, which uses multiple primer and probe sets including H3, pdmInfA, and pdmH1, to subtype any influenza A positives. If a result is positive for a novel influenza A virus including HPAI A(H5N1), CDC must be notified immediately.
Any specimen that tests positive for a novel influenza A virus at the state public health lab is then shipped to CDC's Influenza Division for confirmatory testing. This second layer of confirmation exists because the consequences of a confirmed human H5N1 case are significant from a public health perspective, and confirmation at the national reference laboratory ensures the result is solid before a major response is triggered. CDC also ships to a designated WHO Reference Laboratory in Atlanta. The entire chain is designed to be fast, because speed matters both for patient treatment and for outbreak containment.
From a timing standpoint, RT-PCR at a public health lab can typically return results within hours to a day or two once the specimen arrives. Shipping time from a remote location to the lab is usually the biggest source of delay, which is another reason why contacting your state health department early helps. They can coordinate transport and prioritize processing.
Understanding results: positives, negatives, and inconclusive outcomes

A positive RT-PCR result for H5 from a state public health lab is a preliminary positive. It gets treated seriously immediately, but it goes to CDC for confirmation before it is officially classified as a confirmed human case. Clinically, though, a preliminary positive means you will be managed as a likely case from that point forward.
A negative result is generally reassuring, but it comes with context. The results are interpreted in the context of your exposure and timing, since a negative or inconclusive test can happen depending on specimen quality and when you were swabbed how is bird flu diagnosed. If your specimen was collected very early in the illness, before viral shedding peaks, or if it was a suboptimal swab, there is a small chance of a false negative. If you test negative on an upper respiratory specimen but your illness is progressing and you are seriously unwell, your care team may pursue lower respiratory sampling. Timing matters a lot here. The window for best viral detection in upper respiratory specimens is typically within the first few days of symptom onset.
An inconclusive or indeterminate result usually means the specimen quality was insufficient, or the assay signals were borderline. In this situation, clinicians and public health teams will typically recommend repeat testing with a fresh specimen. It does not mean you are in the clear, and it does not mean you definitely have bird flu. The right move is to stay in close contact with your health department and follow their guidance on whether and when to resample.
Serology adds another layer for retrospective diagnosis. If someone was potentially exposed but did not seek testing during the acute phase, paired serum samples (one taken early and one taken 21 or more days later) can look for antibody responses. This method is less useful for real-time clinical management but important for surveillance and understanding the true scope of exposures in an outbreak.
Next steps after testing: isolation, treatment, and who to call
If you are being tested, you should isolate away from other household members until results come back and the health department advises otherwise. CDC explicitly recommends this precautionary isolation step. This does not mean you have bird flu. It means the risk is low but not zero while testing is pending, and isolation is the responsible default.
On the treatment side, clinicians are instructed to consider starting antiviral treatment empirically while testing is being arranged, especially if you are seriously ill. Oseltamivir (Tamiflu) is the primary antiviral used for avian influenza in humans. You do not need a confirmed positive result before treatment begins if your clinical picture and exposure history are compelling. Waiting for lab confirmation before treating a seriously ill patient would not be the right call.
Here is the practical sequence of what to do if you are concerned:
- Call your doctor or go to an emergency room if you are seriously ill. Tell them about your exposure history upfront, before the visit if possible.
- Contact your state or local health department. They coordinate the testing process and can advise on whether you meet the criteria for H5 testing even before you see a clinician.
- Follow isolation guidance at home until you have results and the health department clears you.
- Do not show up to a crowded waiting room without calling ahead. Alert the clinic or hospital so they can prepare appropriate infection control measures before you arrive.
- If you test negative but symptoms worsen, go back. A negative early in illness does not rule out the diagnosis if clinical suspicion remains high.
One thing worth noting: because this article focuses on testing in humans, the process for diagnosing bird flu in animals is a separate pathway handled by veterinary and agricultural authorities. If you are trying to understand how infection is detected in flocks or individual birds, that involves different testing systems and specimen types. If you need guidance on how to test for bird flu in chickens specifically, veterinary and agricultural testing protocols cover sample types, handling, and reporting requirements. Similarly, how clinicians formally diagnose bird flu, including the broader case definition framework used by WHO, involves layers beyond just the lab test, including epidemiologic linkage and clinical criteria working together.
The bottom line is that if you have a real exposure and real symptoms, the tools exist to test you quickly and accurately. If you meant birds specifically, you can also learn how to tell if a bird has bird flu based on reliable field signs and reporting guidance. The system depends on you making that first call to a clinician or your health department rather than waiting at home hoping it resolves on its own. Do not let uncertainty or worry about being wrong stop you from making contact. Public health authorities would far rather rule out a case than miss one.
FAQ
Can I take a standard at-home flu test and see if it is bird flu?
No. At-home tests and most rapid flu tests cannot reliably determine the influenza subtype, they only indicate influenza A or B. If you have bird exposure plus symptoms, you need clinician-arranged RT-PCR through public health, not an antigen test.
What if my first test is negative, but I still strongly suspect bird flu?
A negative upper respiratory RT-PCR does not end evaluation when symptoms or exposure are compelling. If illness is worsening or you were swabbed very early, clinicians may arrange repeat testing, including a lower respiratory specimen in severe cases, because viral shedding can be harder to detect in the upper airway later on.
How soon after symptoms start can RT-PCR detect H5N1, and does testing later still help?
Best detection in upper respiratory specimens is usually in the first few days after symptom onset. Testing later can still be meaningful if the person is severely ill or if a lower respiratory specimen is obtained, since lower tract viral shedding can persist longer.
If I only have pink eye, do I still need RT-PCR testing?
It depends on the exposure. If conjunctivitis occurs after a relevant exposure to infected poultry, wild birds, or a known human case, evaluation is warranted. CDC-style testing may include both a conjunctival swab and a nasopharyngeal swab, with separate testing rather than pooling.
What is the difference between “preliminary positive” and “confirmed case”?
A preliminary positive means a state public health laboratory detected a novel influenza A virus pattern consistent with H5. Confirmation requires additional testing at CDC (and potentially transfer to a WHO reference lab), so public health treats you as a likely case immediately while awaiting that final classification.
Do I need to test if I had contact but have no symptoms?
Testing can be considered for asymptomatic people with significant high-risk exposure, but it is generally handled through the health department rather than through routine clinical pathways. Your best next step is to call your local or state public health department so they can advise on whether a swab is feasible and appropriate.
Where should the specimen be tested, can a commercial lab do the subtype?
Bird flu subtype testing is handled through state or local public health labs, not typical commercial platforms. Those public health labs run H5-targeted RT-PCR and then forward positives for CDC confirmation using national reference procedures.
Should swabs be combined or pooled to save time?
For key respiratory specimen types, CDC guidance calls for testing certain samples separately rather than pooled, because combining can reduce interpretability when signals are borderline or when only one specimen type contains detectable virus.
If I am hospitalized and already tested negative from the upper airway, what changes?
If you are critically ill, on ventilation, and the upper respiratory specimen is negative, clinicians may obtain a lower respiratory specimen such as endotracheal aspirate or bronchoalveolar lavage. This is done because the virus can remain detectable longer in the lower respiratory tract in severe cases.
What happens if my specimen is “inconclusive” or indeterminate?
An indeterminate result usually means the specimen quality was insufficient or assay signals were borderline. In that situation, the usual next step is repeat testing with a new specimen, coordinated with public health, rather than assuming you are clear.
Will antivirals start immediately while testing is pending?
Often, yes. If you have serious illness and a credible exposure or compatible clinical picture, clinicians may start oseltamivir while arranging testing. Waiting for lab confirmation is generally not recommended in severe cases when suspicion is high.
Is isolation at home necessary if I am being tested but do not have results yet?
Yes, precautionary isolation is recommended while results are pending, since risk is low but not zero. Follow your health department’s instructions on duration and household precautions, especially if you share air with others.
How can I speed up getting tested if I’m worried right now?
Call a clinician and explicitly describe both the exposure and symptoms (or eye symptoms with exposure). If a clinician believes bird flu testing is appropriate, they will contact the state health department to coordinate specimen handling and transport, which is often where delays happen.
How to Test for Bird Flu in Chickens: What to Do
Step-by-step guidance on spotting suspected bird flu, isolating, and what labs do to test chickens safely and quickly.


