Bird flu is genuinely dangerous when it infects a human, but for most people right now the actual risk of getting infected is low. If you want the quick takeaway on how bad it is, the answer depends on both how severe infection can be and how likely you are to be exposed how bad is bird flu. That tension between severity and likelihood is the core of every honest answer to this question. If you want a quick comparison, check how bad is bird flu and how deadly is bird flu side by side. If you want to compare that severity side by side with transmission risk and overall “badness,” see why is bird flu so deadly is the bird flu deadly. The H5N1 strain of bird flu has a historical case fatality proportion of roughly 50%, meaning about half of the people confirmed infected over the decades have died. That is an alarming number. At the same time, the total count of human cases worldwide remains relatively small, and the virus still does not spread efficiently from person to person. So the danger is real and serious, but it is not equally distributed across everyone. Your personal risk depends almost entirely on how close you get to infected birds or animals.
How Dangerous Is Bird Flu? Seriousness, Risk, and Next Steps

Why bird flu is considered so dangerous

Three factors shape how dangerous any infectious disease is to a population: how likely exposure is, how easily the virus infects people once exposed, and how susceptible the general population is. Right now, H5N1 scores high on severity but lower on exposure likelihood and person-to-person infectiousness. That combination keeps it from being a day-to-day threat for most people while still warranting serious attention from public health officials.
What makes H5N1 specifically dangerous when infection does happen is that it can cause severe respiratory illness, including viral pneumonia and acute respiratory failure. The illness is not just a bad flu. The CDC describes a wide spectrum ranging from mild upper respiratory symptoms and conjunctivitis (eye redness) all the way to severe pneumonia and death. Between January 2023 and April 2024, the WHO recorded 889 human cases across 23 countries with 463 deaths. That is not a number you can wave away.
The other reason public health agencies watch this virus so carefully is pandemic potential. If H5N1 or a related strain were to acquire sustained human-to-human transmission, the CDC has explicitly stated it could trigger a pandemic. The virus is already widespread in wild birds and has spilled over into dairy cattle herds, poultry flocks, and a range of mammals. Each spillover is another opportunity for the virus to pick up mutations. That is not a prediction of disaster, but it is a legitimate reason for ongoing vigilance.
How serious is it for humans? Risk by exposure level

For someone with no direct contact with birds or infected animals, the risk of getting infected today is very low. For someone who works with poultry or livestock, handles wild birds, or lives in or travels to an area experiencing an active outbreak, that risk is meaningfully higher.
| Exposure Group | Infection Risk Level | Key Concern |
|---|---|---|
| General public with no animal contact | Very low | No direct exposure pathway |
| Travelers to areas with active outbreaks | Low to moderate | Possible contact with live poultry markets or infected animals |
| Poultry and farm workers | Moderate to higher | Regular direct contact with potentially infected birds or materials |
| People handling sick or dead wild birds | Moderate to higher | Direct contact with infected animals without PPE |
| Caregivers of confirmed bird flu patients | Low (currently) | Human-to-human spread has not been sustained, but monitoring is warranted |
| People eating properly cooked poultry or eggs | Negligible | No evidence of transmission through properly handled, cooked food |
On the food safety question: the CDC and OSHA both confirm there is no evidence that anyone has been infected by eating properly handled and cooked poultry or eggs. Uncooked poultry products or blood have been implicated in a small number of cases historically in Southeast Asia, but standard food safety practices eliminate that risk. You do not need to change your diet.
How bird flu spreads and what that means for your risk
Bird flu spreads primarily from infected animals to humans through direct or close contact. This means touching infected birds or their droppings, being in environments heavily contaminated with the virus (like live poultry markets), or handling infected carcasses without protective equipment. The virus does not currently spread easily between people. The WHO characterizes human-to-human transmission as very limited, and there is no evidence of sustained community spread as of today.
That said, the route of transmission matters for understanding protection. The virus can enter through the respiratory tract (inhaling viral particles) or through the eyes, nose, or mouth after touching contaminated surfaces and then touching your face. This is why eye protection and respiratory protection are both part of the recommended gear for high-exposure workers, not just masks alone.
Wild birds spread the virus to domestic poultry, and from there workers in contact with those flocks carry the highest occupational risk. Dairy cattle in the U.S. have also been affected in recent years, adding another exposure pathway for farmworkers. Each time the virus infects a new animal species, surveillance teams track it closely for signs of adaptation toward easier human infection.
Who needs to be most careful right now
Certain groups face a higher chance of exposure and should take precautions seriously. This is not about panic, it is about proportionate action based on actual risk.
- Poultry and livestock workers, especially those working on farms with confirmed or suspected H5N1 infections in animals
- People who handle wild birds, whether recreationally (hunters, wildlife rehabilitators) or professionally
- Travelers visiting regions with active outbreaks in poultry or animals, particularly areas with live bird markets
- Laboratory workers handling specimens from potentially infected animals or humans
- People with underlying health conditions (such as immunocompromising conditions, heart or lung disease) who have any of the above exposures, since these individuals face higher risk of severe illness if infected
- Caregivers of anyone confirmed or suspected to have bird flu
For workers with occupational exposure, OSHA recommends proper training and the use of appropriate respirators (N95 or better) combined with eye protection when working around potentially infected animals or materials. PPE use is not just a formality: the CDC's post-exposure guidance specifically factors in whether respiratory and eye protection were worn when deciding if antiviral preventive medication is warranted after an exposure.
Symptoms to watch for

If you have had a potential exposure, the CDC says to watch yourself for about 10 days after your last contact with infected animals or environments. The symptoms that should trigger immediate action include:
- Fever or feeling feverish or chills
- Cough
- Shortness of breath or difficulty breathing
- Eye redness or discharge (conjunctivitis), which can appear even without respiratory symptoms
- Sore throat, runny nose, or body aches in combination with a known exposure
Conjunctivitis alone after a bird exposure is worth reporting. It has been one of the more common presentations in recent U.S. cases, and people sometimes dismiss eye irritation as minor. It is not minor in this context.
What to do if you've been exposed or feel sick
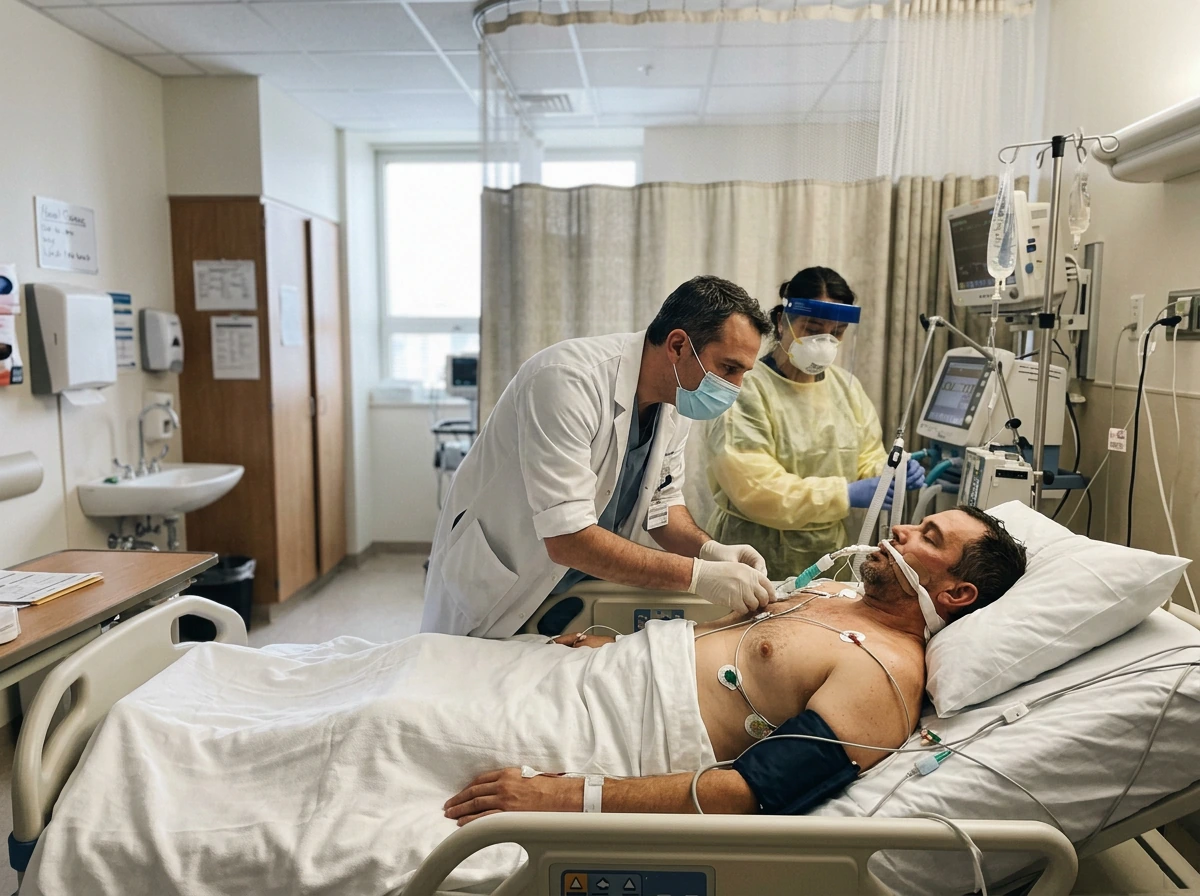
If you have had direct contact with sick or dead birds, infected animals, or environments with confirmed H5N1 and you develop any of the symptoms listed above, do not wait. The WHO advises seeking medical care immediately. Early treatment matters: the CDC notes that early use of antivirals was associated with better survival in global case data, and treatment should start as soon as bird flu is suspected, not only after confirmation.
- Call ahead before going to a clinic or emergency room so staff can take infection control precautions before you arrive.
- Tell the provider exactly what your exposure was: what animal, when, for how long, and whether you used any protective equipment.
- Ask about oseltamivir (Tamiflu) or another neuraminidase inhibitor. The CDC recommends evaluation and antiviral treatment for anyone with symptoms plus a relevant exposure history. Do not let a provider dismiss you without addressing the exposure.
- Contact your state or local health department. If your exposure was occupational or involved a known infected flock or herd, the health department may want to investigate and can guide your next steps, including whether post-exposure antiviral prophylaxis (preventive medication) is appropriate.
- Isolate yourself from household members as much as possible while you are symptomatic and until you get guidance from a healthcare provider or public health authority.
- Monitor yourself for the full 10 days after last exposure even if you feel fine initially, since symptoms can develop over that window.
On the question of post-exposure preventive antivirals: the CDC's guidance is specific rather than blanket. Decisions about giving antiviral medication before symptoms appear depend on the type of exposure, whether PPE was used, how long the exposure lasted, whether the animals involved were known to be infected, and how much time has passed since exposure (the window for considering it is typically within about 2 days). This is why contacting public health quickly matters. The window closes fast.
Practical steps you can take today

For the general public, the practical steps are straightforward. Avoid touching wild birds, especially sick or dead ones. If you find a dead bird, do not handle it with bare hands. Wash your hands thoroughly and frequently if you spend time around animals. Cook poultry and eggs to safe internal temperatures. Stay informed through the CDC and WHO, both of which update their bird flu guidance regularly as the situation evolves.
For higher-risk groups, the bar for action is higher. If you work with poultry, livestock, or wild animals professionally, confirm your employer has a PPE protocol in place and that you are trained on it. Know your local health department's contact number before you need it. If you develop any symptoms within 10 days of an exposure, treat it as urgent and say so clearly when you seek care.
The bottom line is this: bird flu deserves respect, not panic. The severity of disease when infection occurs is real and documented. If you are also wondering about whether it could be dangerous for pets, see is bird flu deadly to dogs as a related consideration. The mortality figures are not exaggerated. That is why many people ask, <a data-article-id="CBB96791-787A-4C9E-BDA3-460300C9FCDB"><a data-article-id="F18F790B-A994-48E4-A8C8-53492418A46B"><a data-article-id="F861F02D-D053-49CE-8A8A-971AA8BF3ADD"><a data-article-id="5C24FC6A-193F-4A58-8745-22B2A9C62397">is the bird flu deadly</a></a></a></a>, and the honest answer depends on how severe outcomes are and how likely infection is. If you are specifically asking whether is bird flu 100 fatal, remember that outcomes vary by exposure and what strain you encounter, so it is better to look at how deadly bird flu can be overall. But for most people living normal lives without occupational or recreational exposure to birds or infected animals, the daily risk remains very low. The situation can change, which is why staying informed is genuinely useful, but right now the people who need to act most urgently are those with direct animal exposure. If that is you, the steps above are not optional.
FAQ
If bird flu is so deadly, why doesn’t that mean everyone is at high risk right now?
A useful rule is to separate “chance of exposure” from “chance of severe illness.” For most people, the exposure route (touching infected animals, droppings, or contaminated environments) is the limiting factor. The virus can be deadly once it infects, but that does not automatically mean a high day-to-day personal risk if you do not have that exposure.
Does living in an area with bird flu automatically make me likely to get infected?
No. The primary risk comes from close contact with infected birds or materials. “Having it near you” matters much less than direct contact, which is why surveillance and worker protections focus on live animal handling, carcass cleanup, and contaminated farm or market environments.
Why does conjunctivitis matter after bird exposure?
Eye symptoms after bird exposure are not “just irritation.” Conjunctivitis, especially after contact with sick or dead birds or confirmed contaminated sites, should be reported and treated as part of a possible bird flu illness rather than something to wait out.
What’s the most common protection mistake for people with occupational exposure?
The biggest common mistake is assuming a mask alone is enough. High-exposure settings can involve droplets and contamination that get into the eyes or onto hands that then touch the face, so guidance emphasizes both respiratory protection and eye protection, plus safe handling and hygiene.
Should I change my diet or worry about food from stores during an outbreak?
Food is generally not the pathway when poultry and eggs are cooked properly. If you are immunocompromised or handling food for high-risk people, the practical add-on is to be extra strict about handwashing after touching raw poultry, avoiding cross-contamination (separate cutting boards and utensils), and cooking through to safe temperatures.
If I might have been exposed, should I wait for test results before contacting care?
Antivirals are most helpful when started early after the right suspicion, not after you wait for lab confirmation. Because the decision to use preventive antivirals can depend on exposure details and timing, contacting public health quickly can matter more than watching symptoms “forever.”
How long after exposure does it still make sense to ask about preventive antivirals?
Timing matters. Preventive antiviral consideration is typically discussed only within a short window after exposure (often around the first couple of days), and it depends on factors like exposure type, duration, whether proper PPE was used, and whether the animals were confirmed infected. That is why the “call quickly” part is so emphasized.
What if symptoms start late, closer to a week or more after exposure?
If you were exposed and develop symptoms within about 10 days, you should treat it as urgent and seek care promptly. The key edge case is that mild early symptoms, including eye symptoms, can show up before obvious severe illness, so “feeling only a little sick” should still trigger contact if you had the exposure.
What should I do if I find a dead wild bird in my area?
If you handle a dead bird, do not assume you can “just wash and be fine.” Use gloves if available, avoid touching your face, bag it if local instructions say to, then wash hands thoroughly after. If you develop respiratory symptoms or eye symptoms afterward, report the bird contact and seek medical advice.
What should I check with my employer before working with poultry, livestock, or potentially contaminated materials?
For workplace safety, ask your employer what respirator type and fit-testing plan you have, whether eye protection is mandatory for your tasks, and how exposures are documented. For monitoring, also clarify the internal process for reporting symptoms and exposures and who to call after hours.

